Does my breastfed baby need supplements over and above her/his breastmilk intake?
A lot of times, infants less than 6 months old are prescribed supplementation as a routine practice, without checking the baby for any deficiency. The most common supplements that are blindly given to babies are calcium, iron, and vitamins. It is important to understand that without a proven deficiency, supplements not only fail to do any good, they actually might do some harm.
Does an exclusively breastfed baby require to be supplemented? Let’s consider the supplementation of each of the above-mentioned nutrients individually.
Calcium Supplements
Breastfed babies get all the calcium they need from their mother’s milk. They do not need additional calcium supplements. Even when a mother is herself calcium deficient, the baby continues to get optimum calcium through breast milk. It is, therefore, necessary for the mother to ensure that she is not sustaining a calcium deficiency. It is important for the mother’s health to maintain optimum calcium levels.
According to the policy of American Academy of Paediatrics, giving additional calcium supplementation to an exclusively breastfed baby does not show evidence of any long-term benefits in terms of bone mineralization.
Iron Supplements
Essentially, all healthy and full-term babies have enough iron stores in their bodies for the first 6 months. Research is also showing that delayed cord clamping at birth can increase the iron stores in the baby’s bodies to last up to an entire year. Therefore, in most cases, there is no iron deficiency and therefore no need for any supplementation.
Human breast milk has lower levels of iron (0.2 to 0.5mg per liter) as compared to cow’s milk. But it is more bioavailable to the human baby. In other words, babies can absorb way more iron from the limited amount of iron available in human breast milk as opposed to the iron abundantly available in cow’s milk. The high lactose levels and vitamin C present in breast milk aids iron absorption. The following table helps understand this better.
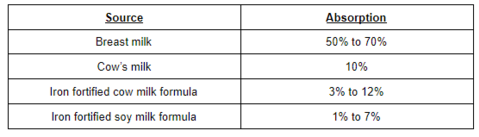
Side effects of unnecessary iron supplementation:
When an exclusively breastfed baby is supplemented with iron without an actual need for it, it can actually do more harm than good. In fact, a review article by Griffins and Abrams, 2001 indicates that – if a baby is basically healthy, iron deficiency in the absence of anemia should not cause developmental consequences. Several studies and research have found the following.
1. Unnecessary supplementation of iron can reduce iron absorption efficiency in the baby –
Research has shown that iron supplements can overwhelm the iron-binding abilities of the proteins in breastmilk. This leads to some of the iron from breastmilk, which was previously available only to the baby, being available to gut bacteria, also. As a result, the baby gets less from the available iron.
2. Supplemental iron can interfere with zinc absorption.
3. Unnecessary iron supplementation can present the following risks –
- Slow growth
- Diarrhea
- Constipation
- Colic
- Changed vitamin A metabolism
When is Iron supplementation necessary?
1. Iron supplementation may be necessary when a baby’s iron levels are checked and are too low.
2. Some babies are at increased risk for anemia. They should be checked for their iron levels and supplemented if necessary. These include the following.
- Preterm babies
- Babies with low birth weight
- Babies who are not breastfed
- Babies born to mothers who have poorly controlled diabetes
- Babies who are given solids earlier than 6 months
3. Increasing a mother’s iron consumption does not increase the iron levels in her breast milk. Therefore, if the baby is deficient, it’s the baby who should be supplemented.
Signs of Iron deficiency:
Low iron levels in a baby can manifest as slow weight gain, pale skin, low appetite, general fussiness etc. When turned into a deficiency, it can potentially lead to developmental delays.
Vitamin Supplements
For healthy full term babies who are
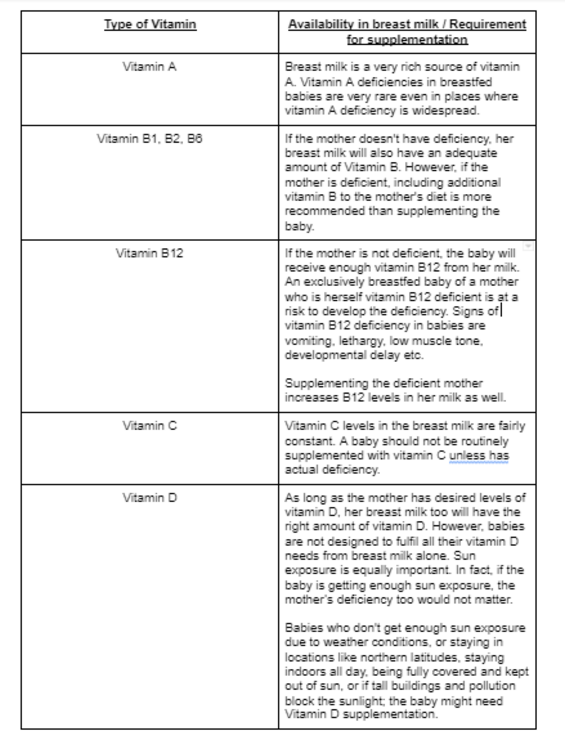

References:
https://kellymom.com/nutrition/vitamins/vitamins/
https://kellymom.com/nutrition/vitamins/vitamin-b12/
https://kellymom.com/nutrition/vitamins/iron/
https://www.llli.org/breastfeeding-info/vitamins-nutritional-supplements/
https://www.llli.org/breastfeeding-info/vitamin-d/
https://breastfeeding.support/iron-breast-milk/
Wish to speak with a member of our team who is a certified lactation professional and also an experienced breastfeeding mother, click on this link.
Medical Advice Disclaimer
THIS WEBSITE DOES NOT PROVIDE MEDICAL ADVICE.
The information, including but not limited to, text, graphics, images and other material contained on this website are for informational purposes only. No material on this site is intended to be a substitute for professional medical advice, diagnosis or treatment. Always seek the advice of your physician or other qualified health care provider with any questions you may have regarding a medical condition or treatment before undertaking a new health care regimen, and never disregard professional medical advice or delay in seeking it because of something you have read on this website.
Disclaimer
We understand and acknowledge that parents and babies can be of various genders on a spectrum of LGBTQI+. Families come in diverse flavours. However, in our articles, for the sake of simplicity and convenience, we will be referring to the breastfeeding parent as the mother and using the female pronouns- ‘she’ and ‘her’ for babies. Babies can be nourished and nurtured in different ways and while we have used the terms breastfeeding and nursing, we recognize that parents can opt to chest feed or finger feed.
We don’t have conflicts of interest and declare, and we are compliant with the WHO code of marketing of breastmilk substitutes and the IMS act.
In case you find any information on this website that needs to be updated, please write to us at info@bsim.org.in






